Wow, 4 months have gone by quickly. April 26th will be the end of 12 weeks after replacement surgery. I haven’t written much about it because my progress hasn’t changed much on a week to week basis. All is going well. I am not back totally; I have occasional discomfort but, overall, I’m doing very well. Everyone says it takes a year plus to get your knee back into the normal range. No matter how quickly I have recovered, I still have 8 more months to go.
Highlights – just being able to walk more than 50 yards. I have a 2.5 mile route through my neighborhood that I have walked several times in the last month, when I have 50 minutes or so to spare. I forget there are three major climbs for me to match the downhills along the way. It is a good effort to get up each one. My leg always feels discomfort by the end of the journey and I wonder … how will it feel tomorrow? I go home and ice it down and the next day, it feels fine / normal for my recovery stage. Although the knee hurts somewhat when I first get up from a chair, within a couple of steps, it is fine, and I notice that I am walking more quickly, closer to a normal pace for me. On Sundays, when I step down from the stage area, I feel almost normal … Yay!
My surgeon, Dr. John Pearce, tells me I am doing well. Thanks, Dr. Pearce – I’m told you are one of the best and I believe it.
I graduated from Texas Physical Therapy Specialists of Austin (Balcones Woods Drive clinic) about 3 weeks ago. Dr. Mark Milligan told me it was time to spread my wings and walk away, they had done their job and I, mine. Kudos to Mark and the staff there. What a great group of people to have guiding me through my recovery / rehab. All along the way, I have met fine people who cared about us, about our health and well-being. My in-home therapist , Sam, recommended TPTSA  and David Browder, DPT, for outpatient rehab. David is the director of the clinic I attended. I walked in the first day – well, I hobbled in the first day and looked around a large room with weights, bikes, incline-machines, tables for joint manipulation and best of all, the beloved ice-machine which ended every workout by circulating icy water around the swollen, inflamed joint to ease results of the workouts. Dr. Mark did an assessment of my knee, put me through a beginning set of workouts and declared that in spite of my character, he would continue treatment. Twice a week, for about 6 or so weeks, I put my knee through a set of exercises to restore flexibility, strength, balance and general confidence in this new apparatus that has invaded my leg.
and David Browder, DPT, for outpatient rehab. David is the director of the clinic I attended. I walked in the first day – well, I hobbled in the first day and looked around a large room with weights, bikes, incline-machines, tables for joint manipulation and best of all, the beloved ice-machine which ended every workout by circulating icy water around the swollen, inflamed joint to ease results of the workouts. Dr. Mark did an assessment of my knee, put me through a beginning set of workouts and declared that in spite of my character, he would continue treatment. Twice a week, for about 6 or so weeks, I put my knee through a set of exercises to restore flexibility, strength, balance and general confidence in this new apparatus that has invaded my leg.
Every visit started with Madi, Laura or Justin putting me on the bike to warm up. 5 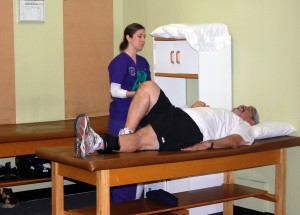 minutes on the bike and we move on to one of the tables. From the table, I would do various stretches, flexes with weights and elastic bands to improve flexing and strength. No, I’m not in these pictures, but you see other clients who didn’t mind getting in the photo. Behind Madi in the photo here is a table with some tan particle-board type material attached to the wall. This is where we did ‘wall-slides’, with my back against the wall, a weight on the ankle, cloth over the shoe to protect the wall from marks and 2 sets of 10 side-leg raises of the left leg then later the right leg too. Can’t end up lopsided … it strengthens the hip muscles, I think, but, these weren’t my favorite exercises 🙁 .
minutes on the bike and we move on to one of the tables. From the table, I would do various stretches, flexes with weights and elastic bands to improve flexing and strength. No, I’m not in these pictures, but you see other clients who didn’t mind getting in the photo. Behind Madi in the photo here is a table with some tan particle-board type material attached to the wall. This is where we did ‘wall-slides’, with my back against the wall, a weight on the ankle, cloth over the shoe to protect the wall from marks and 2 sets of 10 side-leg raises of the left leg then later the right leg too. Can’t end up lopsided … it strengthens the hip muscles, I think, but, these weren’t my favorite exercises 🙁 .
One of the big goals was to get the rotation of the new (left) knee as close to the healthy knee as possible. I was told that my right knee would rotate 135 degrees and when I entered rehab, my 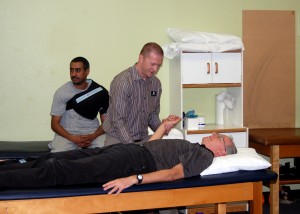 new knee was already back at 115 or so. Earlier I had heard that 120 degrees would be acceptable, but, in my first week, Josh measured my knee at 120 and I thought, good, I’m done with this. Not so fast, my friend. Dr. Mark says, nope, we’re shooting for the whole enchilada, so every session ended with measurements to make sure we were making progress along the way. About 2 weeks from the end, we hit 133 / 135, and then Mark said, ” OK, you’re normal.” Well, he didn’t mean normal like most folks, he just meant that my new knee was rotating as well as the original.
new knee was already back at 115 or so. Earlier I had heard that 120 degrees would be acceptable, but, in my first week, Josh measured my knee at 120 and I thought, good, I’m done with this. Not so fast, my friend. Dr. Mark says, nope, we’re shooting for the whole enchilada, so every session ended with measurements to make sure we were making progress along the way. About 2 weeks from the end, we hit 133 / 135, and then Mark said, ” OK, you’re normal.” Well, he didn’t mean normal like most folks, he just meant that my new knee was rotating as well as the original.
Overall, Dr. Mark was in charge of my rehab, but I had three Doctoral interns from Rocky Mountain University who took turns guiding me on each visit, Josh Rymer, Paul Tripp, and David Kartchner (David is in picture above). A  fine group o’ guys. They were extremely congenial, caring, encouraging, careful and always attentive to how the exercises were affecting me physically. Mark would oversee the session, make sure my knee was manipulated correctly along the way. The PT’s often sat in the center of the room, at the Column of Deliberation, updating files and overseeing everything. Here is Paul and Mark at the column of Deliberation:
fine group o’ guys. They were extremely congenial, caring, encouraging, careful and always attentive to how the exercises were affecting me physically. Mark would oversee the session, make sure my knee was manipulated correctly along the way. The PT’s often sat in the center of the room, at the Column of Deliberation, updating files and overseeing everything. Here is Paul and Mark at the column of Deliberation:  From this vantage point, they could see all the activities ongoing and make sure I didn’t take any shortcuts along the way. They were always watching :).
From this vantage point, they could see all the activities ongoing and make sure I didn’t take any shortcuts along the way. They were always watching :).
One of the more important roles they play is to give encouragement and feedback. I’ve never had a knee replaced. I didn’t know what to expect. I had no idea if a pain was normal or if the screws had come loose in my knee. “Yes, this is to be expected. Yes, most everyone experiences this. What you are experiencing is common. No, your knee will not come unglued nor will it rust in the rain.” Mark told me several times, their goal was to provide good rehabilitation, with minimal pain. I found out my West Texas axiom of “Pain is weakness leaking out” is wrong. All along the way, I was encouraged to use the prescribed medicines to ease the pain because pain can often cause the healing process to slow down or stop. It was good to have wise people leading me through the whole thing (and not my football coaches 🙂 ).
About ten years ago, I tore my Achilles tendon and had surgery to repair it. Because of insurance changes, new job demands, my PT was cut short and I never finished rehabbing. I have regretted it later in years because my ankle and foot pronation were never the same and I tend to roll my right foot and ankle outward when I walk. It makes my shoes wear out in the wrong way. It shows me that after such surgeries, good rehab / PT is very important and following directions for proper healing. Mark gave me some exercises and tools to help with my right ankle and I can tell the difference after adding them to my regimen.
The problem with having good physical therapists is you become addicted to them. It’s so comforting to have a coach, an adviser to give you feedback, keep you on track and working toward your goal. When we started talking about ending the therapy, I had moments of panic. How will I survive? Who will assure me I am getting better? How will I keep up with the various restaurants and eating habits of Josh, Paul and David? I tried to bribe them with fresh bread from my own ovens. I volunteered to sweep the floors and fold all the towels and pillow cases, if only they would let me drop by weekly for a workout. But, alas, I was sent away with a T-shirt and a loud clang on the ‘Gong of Graduation.’ Thanks guys, after all we meant to each other.
But, really, they were a great crew and I recommend them highly if you need some physical  therapy, especially if you are recovering from surgery or some other traumatic event. (In fact friends Jim and Martha Davis are being attended to by this very group).
therapy, especially if you are recovering from surgery or some other traumatic event. (In fact friends Jim and Martha Davis are being attended to by this very group).
In this photo on the left, you see some of the contraptions used for strengthening and for mobility. One thing I would never have thought is the loss of balance with the new knee. With all the trauma to the muscles, ligaments and tendons, they just didn’t work well after the surgery. One of the exercises was to stand on my left leg, balancing for 30 seconds at a time up to two minutes. Very hard to do after my surgery. After a couple of weeks, they complicated it by having me stand in front of the small throw-back / trampoline device on one leg and play catch with myself using a two pound ball bouncing off the mesh. ( It’s in the bottom left of the picture in this paragraph.) Thanks, Mark. I’ll get even with you some day. Actually, I’m not sure I was ever coordinated enough to do this before surgery, so, after … well I got where I could do it for 30 seconds but … come on, man.
But, I did get most of my balance back. How do I know? I found out the other day, I could put my pants on, one leg at a time, without having to sit down. I think it’s working. Rehab doesn’t stop. I continue exercises on my own. Still 8 months of this year long recovery left. We’ll keep in touch.

Jack – thanks for sharing so thoroughly about your knee replacement experience. My 83-yo mother is about to have her’s replaced and I sent her your blog for helping with the unknown and for encouragement.
Thanks, my brother!
Blessings.
Thanks Frank. Glad this could be helpful, there. Now I need to finish writing up my first few days. That’s the biggest hurdle and lots to try to tell. I ran out of steam after telling the first 10 hours :). Give me a shout if she would like to talk about it or I could be helpful in other ways.
Thanks for your kind comments Jack! We’ll miss seeing you. Stop by and chick in every now and then.
Oh, wow, Paul. Thanks for reading my web. I will have to stop in and maybe we’ll go to Rudy’s and give Josh a hard time. You guys were great.
One thing I would never have thought is the loss of balance with the new knee.
Thank you so much for your info, it was very helpful. I had my replacement in sept. I have had trouble with thigh muscles and hip more than my knee from the way I was walking before. I am concerned about some mild pain in my foot, have you experienced that? I have one more p.t. Session, and like you I am nervous about quitting them.
Thank you for your comment. It’s difficult to say about the pain. I had no pain in my foot, that I remember, until my new-found agility and eagerness to renew walking led to long walks and a serious bout of Plantar Fasciitis. That was extremely painful and required a week of little activity and a trip to find some arch supports for my shoes. After 3 weeks of rest and new supports, I was able to renew my exercise but no more road work :).
hi jack I have been looking for people who have had a knee replacement to chat with to hopefully ask if they have experienced any thing such as I am. I had my right knee replaced sept 24, 2013 I was bone to bone (actually both my knees are) and have osteoarthritis in both. the left knee isn’t good.. waiting to do that one therapy is now done. I am 56. my PA says everything looks fine but I am experiencing some things which don’t seem normal to me .have to go back for 6month check in april, but don’t know whether I should contact her for earlier one… and would like to hear if anyone has or is still experiencing them. I am back to work since 12/3 . same retail job for the past 18 yrs.. my knee is still numb on the right side the tendons and or ligaments seem to catch in the front and side of my knee when ..hurts.. and the back of my knee seems to want to give out when getting out of the car or after sitting for a while, then getting up. the PA said its just weak muscles.. my left side of the knee seems to itch a lot (inside the knee?)(which my husband says is a sign of healing?) when I scratch the area it is numb and then the area around my knee tingles like tiny needles poking me. when I get up in the morning and put my foot unto the floor there is tingling and numbness between my big toe people tell me they felt better really quick after the replacement and therapy, but this doesn’t seem to be me. I am slightly over 4months in, she said give it time….am I rushing the recovery ? started going to do excersises in a 90 degree pool a few days a week.. hoping that helps…… would love to hear from you or those with knee replacement/s. with their experience……. just need some confidence , am discouraged.. sorry I wrote so much thanks for the time.. god bless Cat
Hi, Cat. Congrats on the new Knee. I am not a doctor, nor do I play one on TV. That being said, some of your symptoms are familiar, some not. You don’t mention physical therapy. Have you done any of that? After my in-home therapy I attended an excellent PT office and received PT twice a week for a bit and then maybe once a week … I can’t remember the full regimen but I don’t think my recovery would have been the same without it.
I was also bone-on-bone, had been that way for several years and too stubborn to go in. My left knee was replaced and the outside of my knee (left side) is still numb 1.5 years after. My doc told me this was a possibility. It is odd, but not problematic. I have some slight pain sensation when climbing stairs, really only the first couple of steps. It’s like my new knee doesn’t work the same way and it takes a moment for my leg to figure out how to use it. After that, I am fine (our bedroom is 12 steps up). I hate to use the word pain because it isn’t anything bad, but it isn’t just a different feeling, either.
I also remember when I began to workout on my own, I had the fear of my knee buckling backward .. what keeps it from doing that?? It went away and I do a good bit of exercise in the gym now. I don’t have any hesitation to do most things. I don’t try the treadmill at a fast speed, but no one ever accused me of speed, anyway. I prefer the eliptical orbiter for aerobics. I don’t jump :). I can’t speak to your other concerns as they are specific to you. A trainer / PT would be able to answer these with observational experience. I hope this helps.
God Bless you on your recovery.
Jack
Jack, I guess we all are looking for real live humans going through the same things we are. I had left knee replacement on nov 1 and right on dec 15 and have been doing great and for the last week I have had real pain in the left knee (4 mts post) has this happened to anyone else. I guess we are all looking for what is normal, my doc is on vacation! My prayers to all in this boat!
Thanks, DeDe
Wow, DeDe! I couldn’t imagine doing both knees at once. Now I am trying to wrap my mind around both done in 6 weeks. We pray for relief from pain and that it is only a temporary problem. I trust your doc will get back soon. I have a friend who had knee surgery 3 months ahead of me and she experienced pain frequently over the first six months. She is doing great now. That’s the extent of my knowledge.
Blessings
Thanks for the reply, I have reached out to several people and most have pain of some sort or another for a year. I am trying to resume my regular life and I guess I have pushed it a bit much. I am used to being active and am not very patient! Thanks again and many blessings to you!
Thanks for sharing really wonderful info..
I had my left knee replaced 8 weeks ago tomorrow. I have been going to PT 3 times a week. I have 130 degrees and almost complete extension. They say about 1 centimeter left! WOW, how much is that? 🙂 I have some tenderness on the inside and then the next day or so on the outside. Stairs are not an issue and have not taken pain meds for 4 days even before PT (I was only taking them then the last 3 weeks). I am trying to build the thigh muscles and hamstrings now for strength. I cannot stand for a long time, is this normal? Am I rushing into thinking I should be able to do this?
It sounds like you are doing very well. Great job! The range of motion is very important so you are almost there. Some tenderness to be expected, loss of strength and balance was my experience as well so keep building them up. Congrats on getting a new knee and on getting back so quickly..
Jack